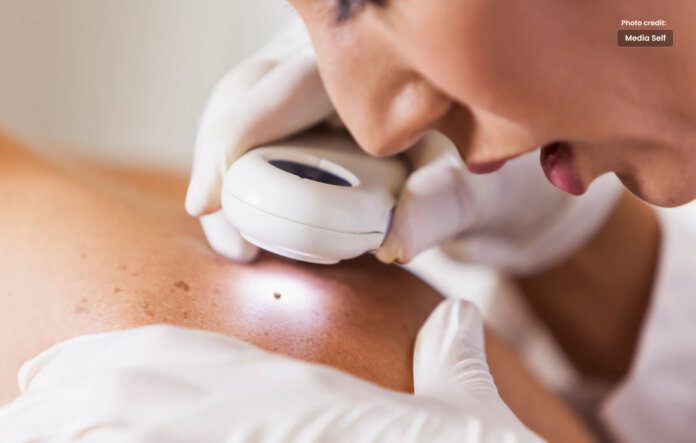
Skin tag removal, known as “acrochordons,” benign cutaneous growth.
The skin tag histology will show a flattened basal cell layer, an attenuated epidermis, and frequently enhanced pigmentation. Loose fibrous tissue makes up the excess mass.
However, it should be recognized right away that patients with obesity, diabetes, metabolic syndrome (MeTS), and those who have a family history of skin tags are more likely to develop acrochordons. Both men and women can get skin tags.
Acrochordons are more prevalent in later life, though they might start to show up as early as adolescence. Skin tags are becoming more common in children and teenagers, according to numerous research.
The latter appears to be related to the worldwide increase in the prevalence of children and adolescent obesity.
On the other hand, following the seventh decade of life, skin tags are uncommon. These lesions typically develop in the axilla, neck, eyelids, and groin—areas where there are skin folds.
The lesions are ovoid growths that are skin-colored, brown, or even red and are frequently pedunculated and linked to a fleshy stalk.
Skin tags typically range in size from 1 to 5 mm, although they sporadically reach 1 to 2 centimeters. Acrochordon are not painful or tender, yet they can still cause problems. Skin tags becoming trapped on clothing or necklaces is a common complaint from people.
The continual rubbing of clothing against skin tags can occasionally cause bleeding or itching.
Skin tags may be more likely to occur in certain hereditary conditions. In patients with tuberous sclerosis and the Birt-Hogg-Dube (BHD) syndrome.
Acrochordons, also known as the “molluscum pendulum necklace sign,” are frequently observed in huge numbers and frequently create “necklace”-like pattern around the neck in addition to other cutaneous and systemic characteristics.
Etiology
- Improper lipid profile
- Diabetes type 2
- Cardiovascular disease
- Obesity
- Genetic components
The main suspect is frequent skin irritation, which is more common in fat people. Acrochordons, in the opinion of experts, are only the result of the skin natural ageing process and subsequent loss of suppleness.
Skin tag formation may be accelerated by hormonal imbalances (such as high levels of the feminine sex hormones progesterone and osteogeny, or high amounts of human growth hormone in acromegaly). Skin tags may also be prone to or triggered by epidermal growth factor (EGF) and alpha tissue growth factor.
Acrochordons have not been linked to infectious aetiologias, but there are anecdotal indications that some viruses may be to blame.
The human papillomavirus (HPV): Researchers have noted a connection between the infection and skin tags in numerous investigations conducted on a variety of patients.
Epidemiology
Frequency: In the general population, acrochordons are known to occur 50–60% of the time.
Sex: According to reports, both males and females have the same prevalence.
Age: Once a skin tag has formed, ageing may cause it to grow larger or more numerous. Nearly two-thirds of people may acquire acrochordons by the fifth or sixth decade, which typically persist until death.
Pathophysiology
A short, thin pedicle connects the bulk to the skin. However, this attachment has a lot of differences.
Most of these lesions likely fall into the seborrheic keratosis spectrum since melanocytic proliferation and nevus cells are not typically seen.
There is, however, some overlap with other disorders such neurofibromas and melanocytic nevi. Some skin tags seem to represent the remaining traces of an earlier melanocytic nevus.
Histopathology
The pedunculated skin lesion histology will show that it has mild hyperkeratotic epidermis and that the dermal stroma has blood vessels of varying diameters.
Acrochordons are typically distinguished from other anamorphs by their flattened, acanthotic presentation or by a “flowery” pattern resembling epithelium.
In addition to lymphatic veins and dilated capillaries, the dermal layer typically contains loosely distributed collagen fibers. Typically, the classic lesion does not show any appendages.
History and Physical
Presentation: Typically, the lesions are pedunculated on a short stalk. The lesions range in diameter from 0.5 to 2.5 mm, and the length of the stalk varies.
The skin tag may be hyperpigmented, which is typically more prevalent, or it may be the same color as the surrounding skin. The groin, axilla, and side of the neck are where skin tags are most common.
The following are general descriptions of acrochordons:
- Small skin tags: Wrinkled papules that range in size from 1 to 2 mm and are most commonly found on the neck and axillae.
- Small skin tags: Single or several 5 mm long and 2 mm wide filiform skin tags that appear elsewhere on the body.
- Extra-large skin tags: Soft fibromas that are typically found on the lower region of the body (groin), pedunculated lesions that may have a baglike, nevoid, baglike appearance
Giant skin tags draw a lot of attention because they are known to cause patients a great deal of pain when they are seen in the axillae and vaginal areas.
Evaluation
A1c, fasting, and postprandial blood glucose levels should all be ordered as part of the patient examination for diabetes mellitus.
The patient lipid profile also needs to be watched over. The patient BMI should be recorded by the practitioner, who should serially monitor it.
Skin tag removal treatment
Skin tag removal is a must for all of the available therapies. The most often carried out operation today is the use of radio cautery in the office. These are some further skin tag removal techniques:
-
Snip excision
-
Cautery
-
Cryosurgery
The CO2 laser or the nanosecond Q-switched Nd: Yag laser are also used to eliminate smaller skin tags. To lessen the pain, some individuals might need a local anesthetic injection or topical treatment. The skin tag little wound normally closes on its own after being removed.
In the majority of situations, the course of treatment entails excision and removal utilizing radio cautery, snip excision, or cryosurgery. However, due to its simplicity and accuracy, radio cautery is preferred by the majority of specialists.
Risks of having a skin tag removal
The excision of skin tags is often a low-risk clinic operation. But when the lesion is removed, it frequently bleeds freely, necessitating pressure and monitoring throughout the surgery. On occasion, electrocautery or silver nitrate coagulation is required.
Rarely, the patient may endure significant bleeding or develop an abnormal infection after the procedure. By thoroughly documenting any prescription or over-the-counter medications the patient may be taking, the doctor can reduce the chance of complications.
This is important since some medications and herbal supplements might affect how quickly blood clots and bleeds.
Multiple Diagnoses
- In rare cases, skin tags-like dermatologic symptoms of neurofibromatosis type 1 exist.
- Skin tags can occasionally also mimic genital warts.
- Hyperpigmented skin tags resemble melanocytic nevi.
- Skin-colored skin tags mimic congenital warts.
- Pincus tumor, a rare premalignant fibroepithelial tumor, may be an option.
- Yet another uncommon but potential differential diagnosis is seborrheic keratosis.
Surgical Oncology
Skin tags are often benign, and after excision, the majority of times the histology reports support this.
Prognosis
If the skin tag is ignored, the frequent friction with clothing and skin folds could cause it to grow in size. The risk of cancer is extremely low or nonexistent for these lesions, but the histological characteristics are unchanged.
Complications
An inflammatory skin tag may twist on its pedicle; obese people frequently have an elevated risk of inflammation.
Problems with Removal
- When a skin tag is improperly removed, scarring may result.
- Removal of healthy skin tissue can occasionally result in cosmoses alterations. Hence the requirement to consult a qualified clinician.
- The location of the skin tag removal may experience minor sensitivity or possibly irritating dermatitis.
- Rarely, if a nerve growth within the skin tag is cut, a neuroma may develop, causing chronic agony for a few weeks or even months.
Patient Education and Deterrence
Skin tags removal are benign lesions, but they may be associated with type 2 diabetes or obesity, therefore patients should be aware of the importance of maintaining a healthy body weight and blood sugar levels.
To avoid skin irritation and friction damage, people with skin tags around their necks should be advised not to wear jewelry.
Additionally, the patient needs to be warned to stay away from wearing constricting or synthetic clothing, both of which might irritate an existing skin tag.
Among Other Things: Pearls
Patients should be urged to exercise frequently, eat a healthy diet, and reduce weight because doing so not only lowers the chance of developing diabetes and obesity but also may help prevent the development of skin tags.
According to certain research, using syndet bars while bathing and applying adequate moisturizer can both prevent skin tags and lessen their local problems.
Improving Healthcare Team Results
Skin tags or acrochordons shouldn’t be regarded as a singular entity because diabetic patients and people with metabolic syndrome are more likely to develop them.
It is crucial to look into these patients for these comorbidities since in young girls in their second and third decades of life, skin tags may be detected in the context of polycystic ovarian syndrome.
If the skin tag removal is simply, the appearance may improve, but if additional testing is skipped, a metabolic issue could go undetected.
Skin tags and metabolic illnesses like type 2 diabetes have been linked in numerous studies, a thorough examination and follow-up care should be standard procedure.
Although skin tags have no chance of becoming cancerous, primary care physicians should be fully aware that they should still order a referral to a dermatologist if they have any concerns about the lesion.
When carried out by professionals, the removal of skin tags is a quick and uneventful treatment. The patient must be persuaded to alter their way of life, nevertheless. Otherwise, the lesions can come back later.
When it comes to prepping the patient, helping during the surgery, caring for the patient post-operatively, and offering patient guidance, a dermatology specialty-trained nurse can prove to be a great asset.
To improve patient outcomes in these situations, the physician or specialist and the nurse must work as an inter professional healthcare team.